By Bhargav Goswami, AIA, ACHA, LEED AP, Principal, Senior Medical Planner
Renee Fiala, AIA, Medical Planner, Tradewell Fellow
Healthcare design continues to improve patient bed floors as designers successfully incorporate the current best practices of the industry. Attention to safety and efficiency are critical issues; however, designing spaces for effective team collaboration and well-being of all building users can have a substantial impact on the overall success of the unit.
Hackensack Meridian Health Ocean Medical Center recently invested $18.5 million into creating a groundbreaking medical-surgical suite on the third floor, above the Hirair and Anna Hovnanian Emergency Care Center. The project team includes EYP, Turner, BR+A and Stantec. Sherri Shafiei, IIDA, of EYP, was the senior interior designer on the project.
Located in Brick, New Jersey, the new Southwest Pavilion is a medical-surgical suite dedicated to elective surgeries, such as joint and hip replacements, bariatric and GI procedures. At 36,000 square feet, the unit tripled in size.
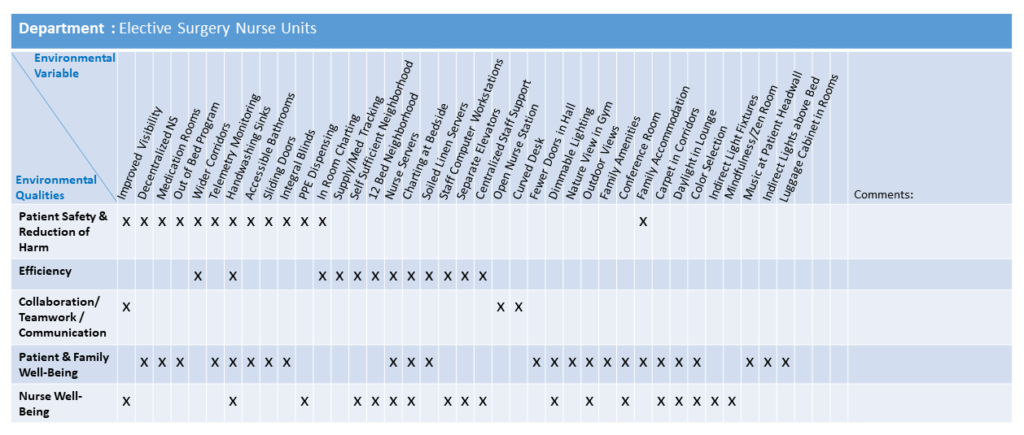
EYP revisited the original Schematic Design layout from five years earlier and made deliberate modifications to address the needs of the new patient population, integrating the most recent best practice concepts. The new layout addresses several categories including: Patient Safety and Reduction of Harm, Efficiency, Collaboration / Teamwork / Communication, Patient and Family Well-Being, and Nurse Well-Being as illustrated in Table 1.
Table 1: Best Practice Categories vs. Improvement Solutions
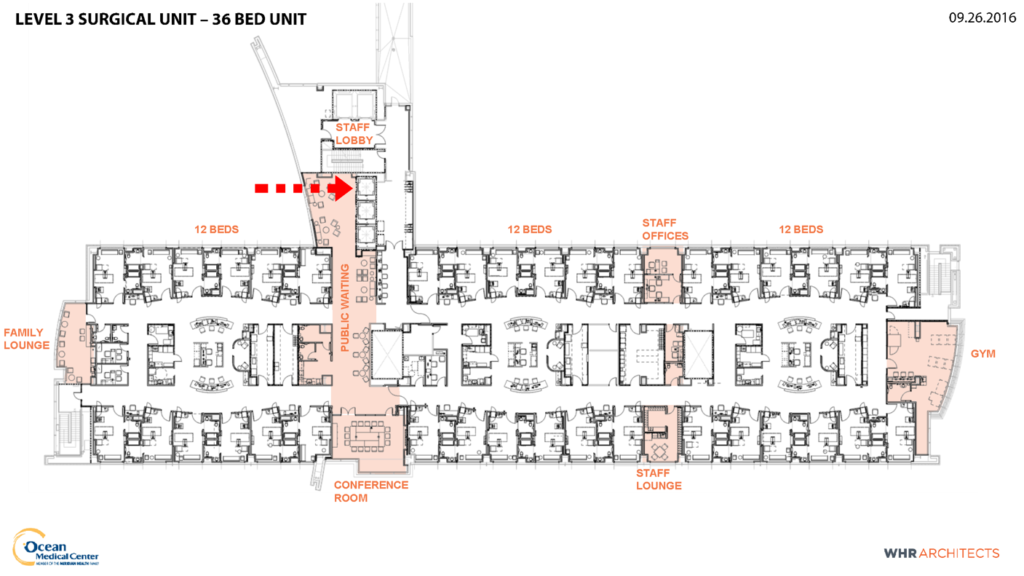
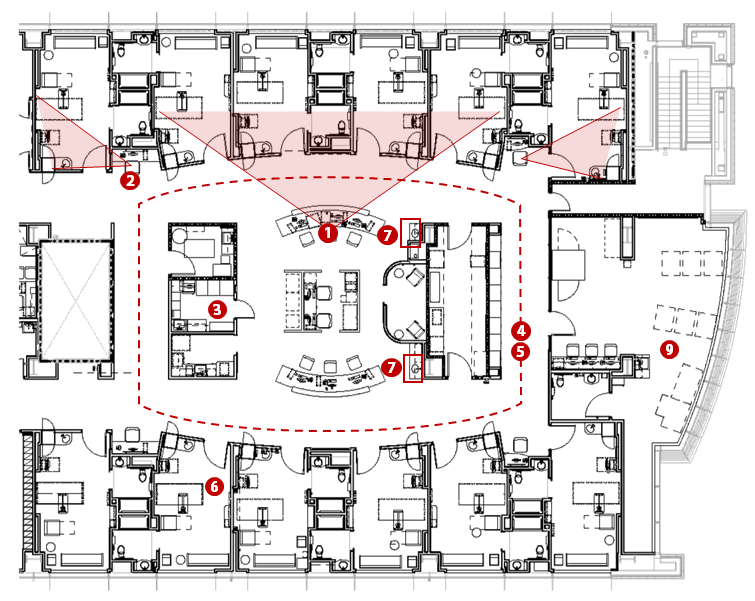
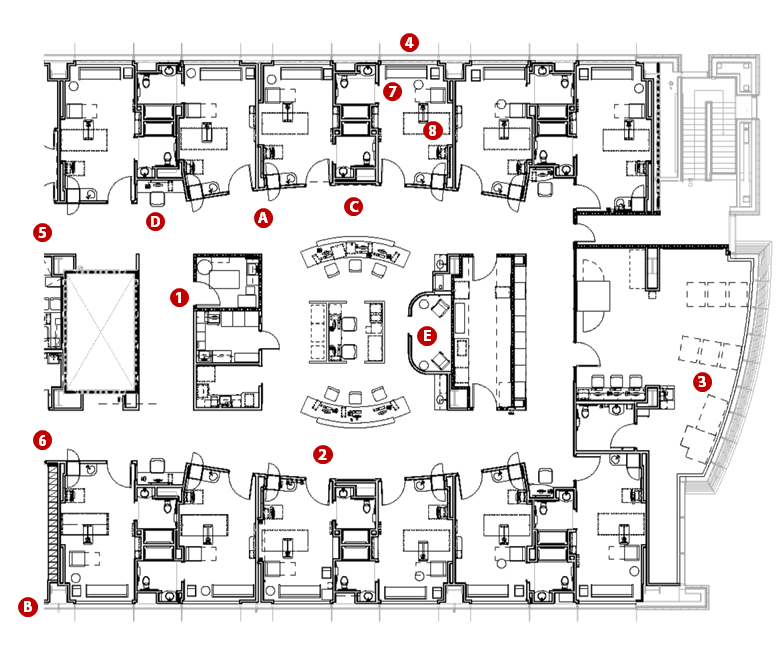
The overall layout of the unit divides the patient beds into three pods of 12-bed neighborhoods. Each pod is designed to be completely self-sufficient to keep staff localized around their patients. The main public and staff elevators, waiting room, and conference room (for patient orientation before surgery) are located between the first and second neighborhoods, and the staff lounge area and offices are located between the second and third neighborhoods for convenient access. See Figure 1. Each neighborhood has a central nurse station and computer work area that is open to both patient room hallways for maximum visibility and communication among team members. There is also a physical therapy gym at one end of the bed floor with floor-to-ceiling windows overlooking the adjacent neighborhood’s tree line. The other end of the floor has an additional family lounge with coffee bar for visitors waiting for a family member to return from surgery.
A. Patient Safety and Reduction of Harm

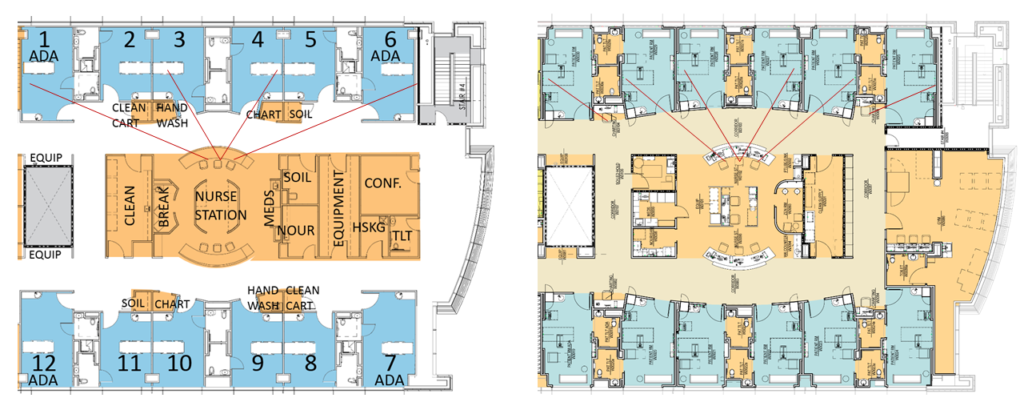
Figure 3: Diagram of Typical Neighborhood Layout, Before (Left) and After (Right)
Medication Rooms were placed at neighborhoods instead of alcoves, to decrease interruptions associated with medication error. Wider corridors promote easier maneuverability for stretchers and use of corridors for mobility therapy. All rooms are wired for telemetry monitoring. Easily accessible handwashing sinks are installed in nurse stations and each patient room. Each neighborhood has four larger rooms to accommodate bariatric patients.
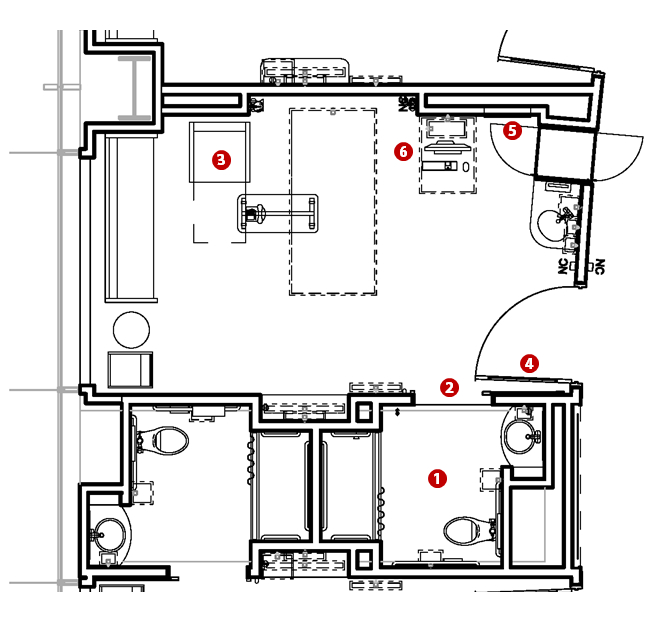
The majority of the issues involving patient safety and reduction of harm occur in the patient room and toilet. Adequate room is needed to be provided for maneuvering frail patients out of the bed and into the bathroom by the nursing staff. Sliding doors with adjacent grab bars provide added patient stability. The headwall has redundant gases and utility access from either side of the patient bed to accommodate the Out-of-Bed patient chair adjacent to the family area to help patients recover mobility/strength faster. Health Risk Management System was installed in each patient room ceiling. The UVC lighting system, clinically proven to eliminate 99.7 percent of pathogens, helps to reduce the number of healthcare-associated infections. Floor mounted toilets in all patient rooms to accommodate the growing bariatric population leads to better safety.
B. Efficiency
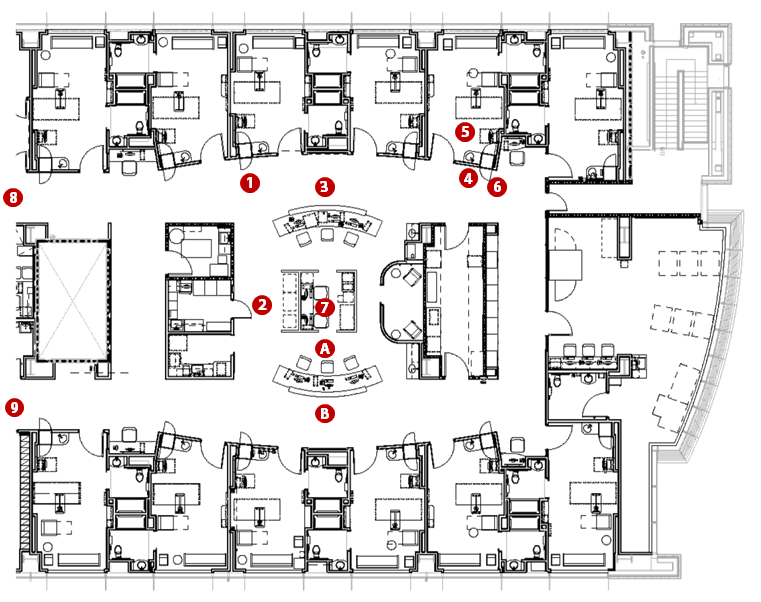
Figure 5: Efficiency and Collaboration / Teamwork / Communication in the Nursing Neighborhood
Increasing efficiency on the unit leads to more time spent with patients. There is improved tracking of supplies and pharmacy/drugs when materials management uses right decrementing software or Par Excellence intelligence. Each neighborhood has its own soiled, clean, medication, nourishment and equipment rooms. Nurse servers in each patient room have access controlled clean supply cabinets above and soiled linen storage below, which allows nurses to walk less and spend more time with patients. Timely access to supplies reduces the physical demands of nursing helping to speed care. Charting computers at the patient bedside keep staff at the point of care. Centralized locations of staff support areas leads to better walking efficiency for staff.
C. Collaboration / Teamwork / Communication
Designing spaces to facilitate interaction among staff members, not only the nursing staff, but also for other team members or physicians working on the unit, contributes to better teamwork and communication. The open nurse station area improves communication. The nurse station extends into the hallway for better lines of sight and observation of the unit. See Figure 5.
D. Patient and Family Well-Being
Improving the patient experience requires rigorous follow-through of detailed design elements that contribute to reduced stress for the patient and family. The enhancement process starts with schematic layouts focusing on providing views, access to nature, and convenient amenities. As the design progresses, details involving specialty lighting and lighting locations, head and footwall configuration, and elements increase the patient control of their environment. Recessed headwall utilities free the wall of institutional equipment behind the patient bed reducing the stress of the patient and family. Bluetooth speakers allow patients to play their personal music at the headwall. Each patient has a device to control the lighting, temperature, window shade, order meals, and call their nurses. The footwall of the patient room has a cabinet to roll in personal luggage and a lockable cabinet to store valuables giving the patient a sense of peace.

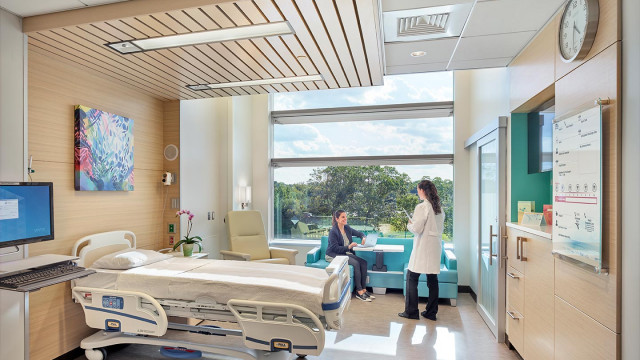
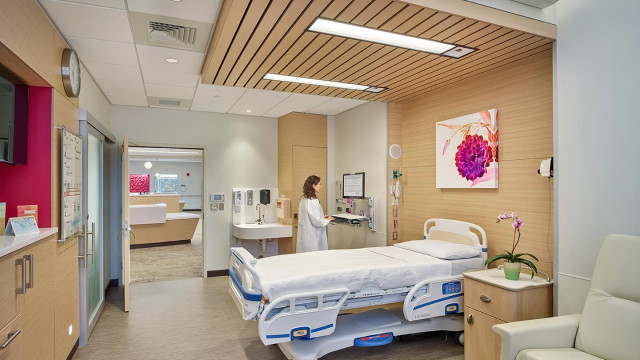
Figure 7: View of the nursing neighborhood.

Figure 8: View of patient room.
E. Nurse Well-Being
Although the patient experience is important, attention to detail in materials and quality of spaces can also positively impact the dedicated nursing staff. Carpet in the corridor helps to reduce noise in the patient rooms and provides better comfort to staff on their feet all day. A Zen room next to the nurse station provides a quiet retreat for staff to de stress and refocus.